Osseointegration Prosthetics
The complete guide to osseointegrated prosthetics for amputees
From surgery and rehabilitation to occupational therapy, physical therapy, exercise and beyond, our goal is helping you achieve your maximum level of independence.
Decades of intensive one-on-one experience with a variety of clients and access to the latest prosthetic technologies have allowed us to identify the perfect approach for a number of cutting-edge prosthetic systems, including osseointegrated prosthetics for arm and leg amputees.
Within this guide are general recommendations and information for those considering an osseointegrated prosthetic system, and insights into who this type of prosthesis is most suitable for. While the information provided here has been collected from years of first-hand experience and trusted sources, almost every case is different.
As such, the material provided here is only intended for informational purposes and should not be considered medical advice. Since every amputee’s situation is different, we recommend an in-person consultation to discuss specific options and to determine whether an osseointegrated prosthetic is the right solution for you.
If you have questions about your unique situation, please reach out to us.
Always Remember: You Have the Power of Choice
 The folks that choose MCOP become members of a much larger community committed to their ongoing health, happiness, and wellbeing – and who wouldn’t want a prosthetic company that’s 100% invested in your outcomes?
The folks that choose MCOP become members of a much larger community committed to their ongoing health, happiness, and wellbeing – and who wouldn’t want a prosthetic company that’s 100% invested in your outcomes?
By choosing to Move Forward with MCOP, you’ll receive:
- The knowledge that you’re working with some of the most experienced prosthetists in the country when it comes to complex or unique limb loss.
- Expert guidance and industry-leading knowledge on the latest prosthetic technologies and activity-specific devices.
- The convenience of an in-house gym and shared services, complete with amputee-specific physical therapy services.
- The added comfort of working with people who truly care.
Over the years, we’ve seen an increasing interest in osseointegration prosthetic options, and the popularity of these systems continues to grow as the technology and surgical procedures rapidly advance. Therapy and rehabilitation for osseointegrated prosthetics is also a bit different than with other prosthetic options. But what exactly is osseointegration prosthetics?
What is Osseointegration Prosthetics?
Osseointegration refers to a direct structural and functional connection between living bone and the surface of a load-carrying implant.
For amputees, it involves a procedure in which a titanium rod is implanted inside of the bone of a residual limb. This osseointegrated titanium rod then serves as the means to attach a prosthetic appliance, and attachment device options are comparable to those prosthetic devices used with traditional socket attachments.
While osseointegrated prosthesis options are relatively new when compared to other prosthetic systems, they’ve quickly gained global acceptance and popularity among prosthetists due to the many unique advantages they provide over other systems, including mobility, strength, and ease-of-use.
How does it work?
Titanium is an extremely biocompatible metal with unique bioactive abilities and has been used for medical applications since the 1950s. The surface of titanium naturally adheres to cells in the body, making it the ideal material for physically bonding directly to bone. Titanium is also resistant to corrosion that could be caused by bodily fluids. 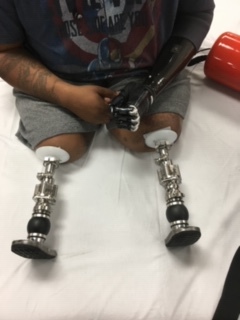
When an osseointegration amputee undergoes surgery, a titanium rod is inserted which forms a strong attachment to the surrounding bone. In many ways, it’s almost as if you’re anchoring an entirely new bone to extend out from the existing residual limb. Meanwhile, there are two main types of osseointegration implants used in limb prosthetics:
- Screw Shaped (OPRA) – Similar to a dental implant, the titanium rod is actually shaped like a screw and is screwed into the bone. These titanium screws aren’t inserted quite as far as press fit prosthesis implants, but screw-shaped implants do require a longer healing time to reach solid integration.
- Press Fit Prosthesis (ILP) – ILP implants resemble a more traditional metal rod without the screw threads and is typically inserted deeper to the bone than an OPRA implant. A press fit prosthesis also has a larger load-bearing capacity, and there are several different types of press-fit prostheses for different applications.
When is it used?
Though popular in dental applications for several decades, osseointegrated implants are a relatively newer option in comparison to conventional socket prosthetic systems. For amputees, the technology and applications of osseointegrated prosthetic systems are constantly improving. At the same time, more patients are switching from externally-worn socket systems to osseointegration systems.
It is worth noting, however, that osseointegration is not an immediate option for new amputees because the necessary surgery cannot occur until about one year after the amputation surgery. If possible, MCOP recommends that patients seeking an osseointegrated system use a socket-based system first. This allows for proper healing to occur, and it also provides the opportunity to first try out a socket system. You may discover that a more traditional (and common) socket-based prosthetic is actually well-suited to meet your needs.
Luckily, you don’t have to rush to make a decision. Whenever you do choose to transition to an osseointegrated system, the process is still the same, regardless of if it takes place today, tomorrow, or five years in the future.
Who uses it?
Most osseointegration procedures are for patients with leg and/or upper-arm amputations, specifically transfemoral (above the knee) or transhumeral (above the elbow). Osseointegration prosthetics are usually only considered after an amputee has already been using a socket-based system and has problems with it. For example, if any of the following issues persist while using a socket system, an osseointegrated system might be a good long-term solution:
- Problems with the socket itself
- Limited mobility
- Discomfort when sitting
- Prosthetic components become easily detached
- Complexities in usage
- General soreness
Problems with the socket itself
Skin irritations, rashes, blisters, and related pains are common issues for patients with socket-based systems. These are caused by a mixture of factors, including an improper fit, perspiration, etc.
Limited mobility
For leg amputees that must stand or walk frequently, it can become uncomfortable or painful to do so with socket-based systems. This limits overall mobility, including the ability to walk long distances and/or run, which can be exceptionally hindering if this type of mobility is essential to your lifestyle.
Discomfort when sitting
For lower-limb amputees, sitting down while the socket system is attached can be extremely uncomfortable, and many people opt to take the socket off as a way to sit more comfortably. Unfortunately, the process of removing the prosthetic several times daily just to sit down is far from ideal.
Prosthetic components become easily detached
When compared to osseointegration systems, socket-based systems can have a bit more of a “loose” feeling. Socket systems are also more likely to become detached during strenuous activities like running, jumping, etc.
Complexities in usage
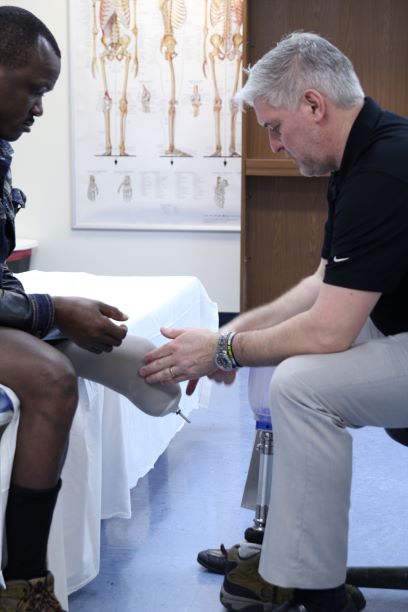 Socket-based prosthetic systems are harder to take on and off because users have to take extra steps to care for the residual limb-stump area. This increases the chances of misplacing a critical component of the prosthetic system, especially if you frequently remove the device and socket for comfort reasons.
Socket-based prosthetic systems are harder to take on and off because users have to take extra steps to care for the residual limb-stump area. This increases the chances of misplacing a critical component of the prosthetic system, especially if you frequently remove the device and socket for comfort reasons.
General soreness
Due to their stability issues, socket prosthetics are more likely to cause improper posture as patients adjust to standing differently or supporting their body weight in an unnatural way. This can lead to all types of health issues or muscular soreness in the amputees’ back, hips, etc. While pain is common with any prosthetic system, if your device is causing additional medical problems beyond the normal soreness, then stability issues related to the socket system could very well be the culprit.
If you or a loved one is experiencing any of the above issues with a current socket-based prosthetic system, it might be time to explore an osseointegrated prosthetic.
Advantages over Traditional Socket Attachments
While osseointegration is not suitable for all amputees, it does offer many unique benefits. For amputees, these benefits should be carefully weighed against the disadvantages of osseointegration. They should also be compared to the pros and cons of socket-based systems. After all, making the transition to osseointegration is a big change that should not be taken lightly.
Here are a few of the key advantages provided by osseointegration.
Strengthen Your Residual Limb
Following any amputation, the non-usage of the residual limb can eventually cause it to weaken because of disuse osteoporosis. Even with traditional socket attachments that fit over the limb, the bone is not loaded upon as it would be naturally. This can lead to decreased muscle volume and weakened bones in and around the residual limb.
A clinic in the Netherlands evaluated bone-remodeling processes and concluded that the bone around an osseointegrated implant becomes thicker and stronger with continued (and typically increased) usage of the area. With the titanium rod serving as an extension of your existing bone, using an osseointegrated prosthetic attachment has been proven to strengthen the residual limb over time. This is because the natural load of the existing bone is restored as amputees begin using it more for load-bearing applications. With this usage, the stump muscles are reactivated and strengthened, which helps to further stabilize the nearby bone and promote fusion between the implant and the bone.
Eliminate Certain Skin Issues
One of the primary drawbacks of traditional socket prosthetics is the unpleasant process of conditioning the skin and tissues around the residual limb. Even when the skin becomes appropriately formed and toughened, rashes, blisters, pressure sores and other issues are still common and, as a result, an amputee will often limit their prosthetic usage.
Osseointegrated prosthetics don’t cause the same types of skin irritation issues because the skin itself is not wrapped up to receive a socket device. Instead, the structural support for the prosthesis is reliant upon the bone structure in which it is attached. When skin issues are reduced, the amputee is more likely to get additional usage out of their prosthetic system.
Easier & More Efficient to Use
Depending on the amputation level, traditional socket attachments are typically a bit more cumbersome to attach, use and detach when compared to an osseointegrated prosthetic system. This is partially due to various socket-related attachments and accessories needed for a comfortable fit (sleeves, wraps, etc.) during usage.
For example, a 2011 study of 22 osseointegrated prosthesis patients in comparison to socket-based devices showed that patients with lower-limb amputations:
- Nearly doubled their prosthetic usage (measured in hours per week)
- Walked significantly faster and farther than before
- Used 18% less energy while walking
- Reported improved quality of life
Ease of use and usage efficiency are also closely linked to enhanced stability and mobility.
Enhances Stability & Mobility
In lower limbs especially, osseointegration offers more overall mobility and stability which helps with walking and standing. The amputee’s natural standing posture is often restored with this weight-bearing advantage, as is the intrinsic stability.
Osseoperception
Osseoperception occurs when a patient regains their proprioception, which is the unconscious perception of the position of the body, movement and spatial orientation in relation to the external environment. This means that patients regain some of their ability to naturally feel things, such as sensing the surface characteristics of something they are walking on, like grass, carpet or uneven pavement. This promotes safer and more confident movements, even in unfamiliar areas or dim light.
Disadvantages
An osseointegration prosthesis is not right for everyone, and sometimes it’s the disadvantages that sway an amputee to continue with socket prosthetics. Before any amputee considers an osseointegrated system, they should first understand some of these disadvantages.
Lengthy Rehabilitation Time
As previously mentioned, the osseointegration process cannot begin until about one year after the initial amputation surgery. For this reason alone, amputees should start out with a traditional socket-based system after their amputation – otherwise, they would be living without any prosthetic. Still, using a socket system involves its own unique rehabilitation and therapy procedures separate from the therapies used when undergoing a transition to an osseointegrated prosthetic.
Even so, osseointegration surgery can sometimes involve a much longer recovery and rehabilitation time frame depending on the amputation level, amputee bone structural makeup and the type of osseointegration implant. Before the new prosthetic system can be fully utilized, the bone needs to completely fuse to the titanium rod to form a strong bond. Forming this bond takes time, during which load bearing is steadily introduced to ensure the residual limb strengthens properly.
From the initial implant surgery date to the return of full strength and mobility, the entire process can take anywhere from 2 to 12 months or longer, with full weight bearing at anywhere from six weeks to 12 months.
Additional Risks
Though the benefits do outweigh the risks, there are still some unique complications associated with osseointegration surgeries and usage, including putting amputees at a higher risk for infection and bone fractures.
Infection
The possibility of infection is one of the more prevalent risks associated with osseointegration, and it’s not just related to the surgical procedure alone. The implant itself has to protrude through the skin and the tissues between the titanium, meaning the outer skin remains partially exposed for an indefinite period of time. As a result, people with osseointegrated systems must practice good hygiene to keep that area clean. Fortunately though, all that’s required to significantly reduce the risk of infection is regular bathing/showering – nothing that the typical adult isn’t already used to.
People with osseointegrated systems should also avoid any activities that increase their risk of infection. This includes avoiding activities such as swimming in pools, lakes, ponds, oceans and other bodies of water. However, there are ways to seal off the area with liners or custom covers should one wish to continue swimming.
Fractures
With this type of bone integration, fracturing the residual limb bone is also a risk with potentially devastating consequences. Especially for lower-limb amputees, a fracture to the femur or humerus, where the titanium rod most commonly inserted, can create a complicated healing and rehabilitation scenario. The patient’s healing process must be carefully monitored so as not to compromise the strength and positioning of the implant.
Luckily, implant manufacturers commonly utilize safety devices that allow the prosthetic to break away from the implant when extreme or unusual torque is applied. It’s similar to snow ski bindings that are designed to detach from the ski boots when a person’s legs/skis become twisted or are torqued excessively.
Because of the potential implications stemming from a bone fracture around the titanium implant, high-impact activities are not permitted at all. Even though the osseointegrated implant provides a better feel and more natural physical sensations, excessive running and jumping is strongly discouraged because fractures pose such a serious risk.
Additionally, because of the high-risk and implications with a bone fracture, osseointegration is not suitable for individuals who weigh 250 lbs or more.
Preparing for your Osseointegration Prosthetic Transition
For any amputee, a new prosthetic system is a big change. So, before any osseointegration surgery is scheduled, you must first determine (with the help of a doctor) if you’re a suitable candidate for this type of prosthetic system. If you are a recent or soon-to-be amputee, the earliest you can have osseointegration implant surgery is one year after your amputation procedure.
Also, if you’re already using another form of prosthesis, then it might be possible to continue using the same or similar device in the future. But, you should first discuss this with your prosthetists as it could affect insurance coverage and the type of device-ready attachment that is connected to the titanium implant.
Insurance
Of course, making sure your insurance will be approved beforehand is a must. So, before any procedure is scheduled, you’ll have to navigate the pathways of obtaining the proper insurance coverage for your device. If you have a work-related injury, your team can work with your workmen’s compensation case manager to obtain the best device for your needs. Whether you have private or government insurance, VA, Tricare, or Medicare/Medicaid, most insurance companies offer options for osseointegrated prosthetics.
Following this decision, prosthetic insurance experts will work to obtain pre-authorization from your insurance regarding the products that are best suited for your lifestyle. It is also important to have your team check your benefits to make sure that there are no exclusions in your insurance policy.
Talk to a Prosthetic Insurance Expert
Pre-Surgery Conditioning
As opposed to preparing for a socket prosthetic, where the pre-surgical physical therapy is a central focus of the overall process (immediately following amputation surgery), preparing for osseointegration surgery is not as intensive since that initial conditioning phase has usually already passed and the stump muscles have been conditioned. However, the conditioning and rehabilitation exercises used with other prosthetics are certainly beneficial when preparing for an osseointegrated prosthesis.
Osseointegration Surgery
There is no way around it: bone surgery is absolutely necessary. The surgical procedure involves inserting a titanium rod directly into the inside of the bone of your amputated limb. If needed, the length of your stump bone could be altered in the surgery and the surrounding soft tissue corrected.
Depending on whether you have an OPRA or ILP prosthetic, the surgery specifics and rehabilitation timeframes can vary. Whether it’s a screw-shaped or press-fit prosthesis, once the rod is fully inserted into your residual bone, a small separate skin incision is made to allow the surgical team to connect an osseointegration adaptor, which will later connect to your chosen prosthetic device.
This skin penetration point is called a stoma. The stoma incision area will naturally drain and you should expect a small amount of discharge during early recovery. In-hospital recovery time can range, but typical stays are around 3 to 5 days. During this time, you’ll receive instructions on how to clean and care for the stoma area. During your first few weeks of recovery, MCOP prosthetists will prepare your prosthetic attachment that will connect to the osseointegration implant.
Post-Surgery Rehabilitation
One of the most critical phases of your osseointegration transition is the months following surgery. This is when you’ll work daily to strengthen the bone and surrounding tissues and condition them for future usage. For the first few weeks, MCOP therapists, rehab specialists, and prosthetists will work closely with you every day to develop a rehabilitation plan that gradually increases your strength and prepares you for living with your new osseointegrated prosthetic system.
Everyone’s rehabilitation plan is different, but you’ll learn how to:
- gradually increase the load to your prosthetic,
- connect and disconnect your prosthetic device,
- walk with crutches (for lower-limb amputees),
- keep the area clean,
- use the new prosthetic system during this critical recovery phase.
Depending on your amputation level and the type of osseointegrated implant, this intensive daily rehabilitation could last up to 6 weeks initially, but patients should continue their daily exercises for several months as they gradually introduce more load-bearing activities. As mentioned earlier, the healing timeline is quite different for OPRA and ILP type implants.
With the OPRA type of implant, full load-bearing activities cannot begin until 6 to 12 months. ILP implants have a larger load-bearing capacity and amputees can usually introduce full load-bearing activities within a few weeks after surgery.
Regardless, the rehabilitation process is not to be taken lightly, and patient perseverance is key to reaching your physical potential with the new prosthesis. Many patients experience extreme muscle pains for up to a year after surgery, especially for those who’ve begun using a new system that engages muscle groups that weren’t previously in use. This is normal, but if pain persists well past your full load-bearing threshold, you should talk with a medical professional.
Additional Information
As you can see, similar to other prosthesis options, determining whether osseointegration is the right solution for you is dependant on your unique amputation situation and your personal preferences.
What are your goals? Let’s talk about how to reach them together!



