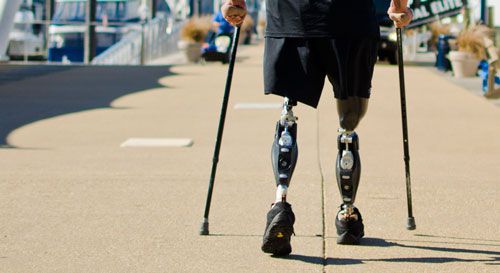
Pelvic Amputation
What is a Hemipelvectomy?
A Comprehensive Guide for Lower-Limb Amputees Preparing For, or Recovering From, a Hemipelvectomy
The Hemipelvectomy Surgery & Recovery Process
From the earliest stages of preparation to the lower-limb surgery itself, then all the way up to postoperative physical therapy and rehabilitation, our skilled team of prosthetists and orthotists are committed to helping hip and pelvis amputees #MoveForward to continue living a happy and fulfilling lifestyle.
From the very beginning, we work closely with clients facing a wide variety of mobility challenges related to lower-limb amputations, including individuals who’ve had an external hemipelvectomy surgery procedure in their lifetime – whether the operation was last week or 20+ years ago.
The combined dedication of our own staff and our physical therapy partners can provide hip and pelvic amputees with all the tools and training they need to meet their mobility goals. Together, we work to discover their unique lower-limb prosthetic requirements, then locate the appropriate prosthetic devices to help them better recover from the challenges associated with pelvic amputation.
Below, you’ll find a comprehensive guide outlining our process of getting hemipelvectomy amputees back to peak mobility levels, the basics of what a hemipelvectomy is, and what to expect with the surgery and postoperative recovery. Wherever you are in your personal journey, we hope that you find this information useful and that it helps you visualize a clearer path toward achieving your personal goals as a hemipelvectomy amputee.
So, what is a hemipelvectomy?
What Is a Hemipelvectomy?
One of the rarest types of lower-extremity, above-knee amputations, hemipelvectomy surgery procedures involve a removal or resectioning of some part of the patient’s pelvis (sometimes as much as half of it). This procedure is typically carried out for the treatment or elimination of the most dangerous conditions and diseases, the most prominent being localized tumors or cancers that have spread to the pelvis and have not been responsive to other forms of treatment such as radiation therapy or chemotherapy.
Traumatic Hemipelvectomy
A hemipelvectomy might also be performed in the wake of serious trauma or an accident that leaves one’s pelvis irreparably damaged. In these cases, the hemipelvectomy amputation is referred to as a traumatic hemipelvectomy. As its name might imply, a traumatic hemipelvectomy should always be carried out as quickly as possible following the accident in order to save the patient’s limb – and, in some cases, life.
External Hemipelvectomy
An external hemipelvectomy involves resectioning of bones within the pelvis, as well as the amputation of the whole leg on the affected side. This process is generally followed up later on with the fitting of a custom hemipelvectomy prosthetic.
How Hemipelvectomy Amputations Differ from Hip Disarticulations
When discussing the basics of the hemipelvectomy, we believe it’s also worth clarifying the difference between this and another lower-extremity amputation known as “hip disarticulation,” as these two are sometimes confused despite their differences.
Hemipelvectomy amputations and hip disarticulation amputations are somewhat similar procedures, so it makes sense why the two can be easily confused from time to time. After all, they both involve the removal of the three lower limb joints (hip, knee, and ankle), and they are both commonly performed as a result of trauma, tumors, or life-threatening infections.
However, the main distinction between the two is that a hip disarticulation removes the entire lower limb through the hip joint, while a hemipelvectomy removes the entire lower limb at the hip level plus a pelvic amputation. As a result, hip disarticulation amputees still have their ischium, the bone that bears weight and allows us to sit, which also serves as a stable area for mounting sockets to support a lower-extremity prosthetic system.
Meanwhile, hemipelvectomy amputees do not have their ischium left on the side where their amputation was performed, which forces their weight to be shifted through the soft tissue surrounding the hip and pelvis on the other side where the ischium still remains.
Because of this loss of the ischium on one side, our staff members spend a lot of time working with hemipelvectomy amputees to ensure their sockets are fitted in the most ideal fashion to provide both comfort and stability to ultimately maximize their mobility potential.
Our team has vast experience with replicating the complex joints of the hip and pelvis with a custom-designed sockets to support a series of technologically advanced prosthetic devices for not only hemipelvectomies, but all types of amputations.
What To Expect From Your Hemipelvectomy Surgery Procedure
Before Your Pelvic Amputation Procedure
Well before your pelvic amputation procedure, you’ll start with all the necessary preoperative preparations, including an appointment with your surgeons that will involve, amongst other things, some in-depth discussions on the upcoming procedure and its possible outcomes.
These discussions will cover a wide range of topics, including everything from the location of your tumor to the severity of your disease or disorder – plus any associated risks or complications.
All of these things are highly circumstantial and will vary greatly from patient to patient, making them essential things to discuss with your preoperative team, which will include professionals from a multitude of disciplines such as surgeons, nurses, physical therapists, nutritionists, plastic surgeons, case managers, and more.
Falling in line with informed consent requirements, these discussions could cover a little bit of
everything, including education on postoperative complications such as loss of bowel and bladder functions, impaired skin integrity, and more.
Like any major surgery, you’ll also receive a full medical workup prior to your operation. You’ll also be informed of any essential dietary restrictions for the days leading up to the surgery, which might restrict you to a clear liquid diet for a designated length of time or to follow necessary bowel-cleansing procedures to reduce the risk of contaminating the wound from the anus.
Navigating Insurance
Finally, you’ll want to address any insurance- and/or billing-related matters as early as possible, which is true when facing any upcoming amputation (or any major surgery at all, for that matter). To help you navigate these potentially tricky billing, insurance, and legal support matters, our team is always on hand to provide a wide range of assistive services for our clients and their families. Find out more about how our certified prosthetists can advise and assist you with your insurance preauthorization, claims, worker’s compensation, disability insurance claims, and more.
During Your Pelvic Amputation Procedure
A standard hemipelvectomy is performed by making a large incision either in the perineum or at the back of the body (where the ilioinguinal nerve is located). If the operation is performed to remove a cancerous tumor, then the tumor will most likely be sent to a lab for assessment. Depending on the results of the analysis, then more bone and tissue samples might be removed and examined until the samples finally come back clean.
After this portion of the hemipelvectomy is complete, the surgeon can begin reconstructing the affected body part, usually through an allograft (the transplantation of an organ or tissue from one person to another person) or an autograft (transplanting bone or tissue from one spot of a person’s body to another part of his or her own body).
Surgical reconstruction is standard following any lower extremity amputation. This will usually involve a skin-transplantation graft or flap procedure to recreate the pelvic area and protect the remaining structures – while also protecting any attached metal screws, plates, or other sensitive materials.
After Your Pelvic Amputation Procedure
Immediately following the procedure, postoperative care will be provided for varying lengths of time within the hospital or intensive care unit. A thorough surgical assessment will also be implemented to reduce or treat any possible wound infections or necrosis and further ensure your health and safety before you can leave the hospital grounds and continue recovery at home.
Post-Operative Hemipelvectomy Resources
Of course, finding a prosthesis following a hemipelvectomy-related limb removal is a major priority, but you’ll also want to keep in mind the fact that any lower extremity amputation is as much a physically challenging procedure as it is a psychologically challenging one. With that said, finding the right physical and occupational therapists, continuing your follow-up care at an outpatient clinic, and staying up to date with routine blood work and tests will all work wonders when it comes to coping with these emotions in a healthy and productive way.
There is also an abundance of support groups and resources, both online and in your community, that can provide opportunities for open dialogue and education as you transition back into daily life. Some of these groups and resources include:
- The Amputee Coalition of America’s Limb Loss Resource Center, which allows visitors to sort through the myriad resources the Coalition offers, including a vast library of articles and links, as well as lists for in-person events and organizations.
- Supportgroups.com serves as a great resource for people in search of an online support group, and their https://amputee.supportgroups.com/ forum is a good hub to read about other amputee’s personal experiences, challenges, and accomplishments – or to post your own.
- Achilles International is a worldwide organization whose mission is to enable people with all types of disabilities to participate in mainstream athletics through a series of programs, national chapters, informative newsletters, and other initiatives.
- Adaptive Adventures is a nonprofit dedicated to improving the lives of people living with disabilities through fun outdoor recreational events taking place throughout the country.
- The I-Can Child Amputee Network is an internet mailing list dedicated to providing information and support contacts for the parents of children with absent or underdeveloped limbs.
Finding the Right Hemipelvectomy Prosthesis for You
When it comes to prosthetic options for pelvic amputations – or any lower extremity amputations, for that matter – the highly trained team at MCOP can help steer you down the right path. Not only can we inform and educate you about the latest and most advanced prosthetic technologies and manufacturers, we’ll also work closely with you to find options that meet your exact needs – while also showing you how to use them.
In our clinical experience, hemipelvectomy amputees can be great candidates for powered prosthetic devices. For example, Ottobock Helix Hip offers maximum security and function for a range of daily activities by mimicking the pelvis’ natural three-dimensional movement patterns in the stance and swing phase. It also reduces the risk of falling and improves posture while sitting. Combined with other powered prosthetics such as the Össur Power Knee, Össur Pro-Flex XC ankle, or iWalk BiOM Foot, hemipelvectomy prosthesis can offer a supreme level of control and natural mobility.
Ottobock Helix Hip Joint System
Ottobock’s Helix 3D Hip Joint System empowers pelvic amputees to walk safely and comfortably after a hemipelvectomy. With a wholly unique joint design, this high-tech hip replacement replicates the natural gait cycle by allowing for three-dimensional and safe movement.
Many of our clients who use the Helix 3D Hip Joint System comment on how easy it is to initiate swing movements thanks to the system’s integrated expansion swings and miniature built-in hydraulics.
We find this product to be much better than conventional hip joint systems, which typically only allow for restrictive, one-dimensional forward-and-backward movements. With the Ottobock Helix 3D Hip Joint System, users are given greater control over every aspect of their mobility, whether they’re taking a walk down the street, completing a physical therapy session, or simply putting on their shoes.
Össur Power Knee
 For external hemipelvectomy clients, we find that some of the more technologically advanced devices do indeed offer the best mobility options by replicating the movements of the knee, another complex joint. Combining power, safety, and endurance, the Össur Power Knee is unprecedented in function and performance. For hip and/or pelvic amputees, it provides superior powered-stance stability to compensate for lost muscle function.
For external hemipelvectomy clients, we find that some of the more technologically advanced devices do indeed offer the best mobility options by replicating the movements of the knee, another complex joint. Combining power, safety, and endurance, the Össur Power Knee is unprecedented in function and performance. For hip and/or pelvic amputees, it provides superior powered-stance stability to compensate for lost muscle function.
The built-in PowerLogic Workbench software enables our prosthetists and physical therapists to monitor clients and give real-time visual feedback in regards to how they are using the device and optimize the device aspects that will improve stability and mobility for each individual. Clients can also easily report on their performance and progress, allowing for convenient documentation and tracking over time.
Össur Pro-Flex XC Ankle
The Össur Pro-Flex XC ankle is one of our most popular dynamic prosthetics for hemipelvectomy amputees. It allows users to keep their long-term healthcare costs low and prevents the need for future surgeries or amputations by reducing the hard load on your remaining joints over time.
The Pro-Flex XC also uses innovative pivot technology to reduce south-side steps, allowing uses to experience a comfortable form of mobility that closely emulates natural foot movement. For amputees who want to enjoy activities from regular day-to-day to intensive jogging and hiking, the Pro-Flex XC makes for an ideal lower-limb prosthetic.
iWalk BiOM Foot
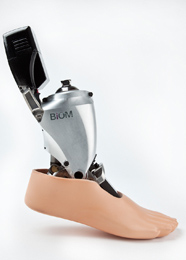 The iWalk BiOM Foot enables hemipelvectomy amputees to regain a natural gait. With each step, it provides a powered push-off to propel the wearer forward. The BiOM Foot is the only prosthesis in the world that does not depend on the wearer’s energy, as it mimics the functions of the calf muscles and Achilles tendon.
The iWalk BiOM Foot enables hemipelvectomy amputees to regain a natural gait. With each step, it provides a powered push-off to propel the wearer forward. The BiOM Foot is the only prosthesis in the world that does not depend on the wearer’s energy, as it mimics the functions of the calf muscles and Achilles tendon.
Users of this unique lower limb prosthetic device will experience natural walking mechanics and increased stability, mobility, and confidence.
Custom Design Systems
We can even create custom prosthetics that give you unmatched functionality for comfortable all-day wear, which can work wonders on your road to recovery. In fact, research and our own years of first-hand experience have shown that wearing your hemipelvectomy prosthesis for longer periods of time has numerous long-term health benefits, including a reduced risk of scoliosis, back pain, deformation and shoulder injury, and a lessened need for future surgeries. And, it is these devices’ ability to mimic natural muscle and joint functions that provide their long-term health benefits.
However, before you can feel comfortable wearing your hemipelvectomy prosthesis for longer periods of time, you need to find a hemipelvectomy prosthesis that’s comfortable! That’s why we always attempt to strike a perfect balance between control and comfort with our unique socket designs, allowing for easy adjustments throughout the day and a much greater level of wearability that our customers love.
Want to Work With Our Team?
Whether you need preliminary assistance with planning things and setting up a pelvic amputation consultation, or if you’re in the recovery stage and are looking for the right hemipelvectomy prosthesis to help you #MoveForward more confidently, we’re always here to help – just as we have been for nearly two decades now.
No matter what, you’ll always receive high-quality, individualized care from our world-renowned team of lower-extremity prosthetic and rehabilitation experts. We’ll do our best to ensure you receive the most effective care, coupled with access to the most advanced prosthetic technologies and devices, all so you can get back to living your life to the fullest as easily as possible.
The next step in your personal recovery journey starts as soon as you contact us. We’re waiting to hear from you!